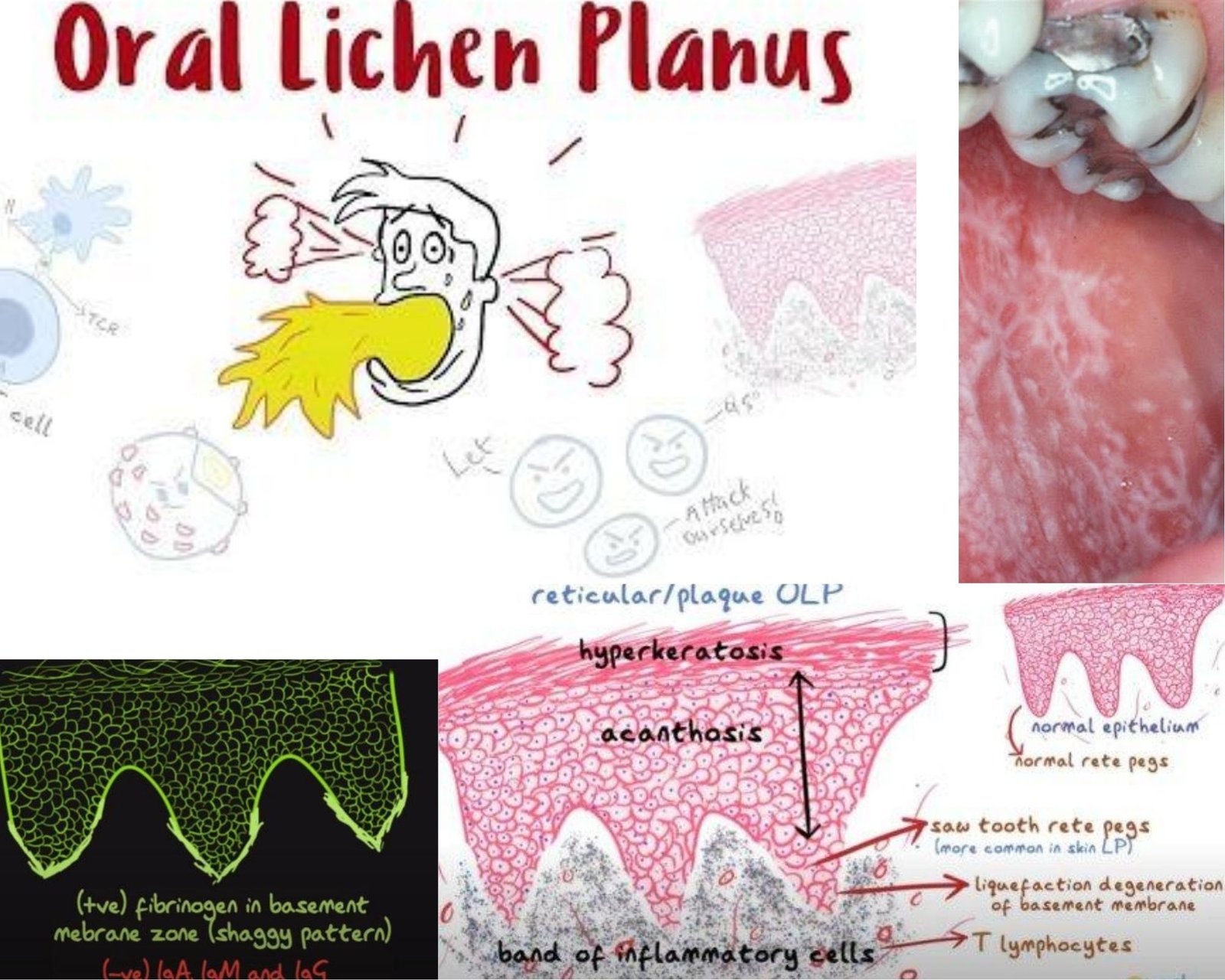
LICHEN PLANUS. Most of us are sure to across this interesting term when we look through information regarding auto-immune disorders. The term is itself inspired by the lichen plant that usually covers rocks and trees in a mossy, web-like fashion, similar to the disorder’s clinical appearance.
It is a chronic immune disorder that can affect the skin, oral mucosa, scalp, genital mucosa, and nails. Oral lesions have often been seen in the absence of skin lesions. It is in fact, one of the most common dermatological diseases to affect the oral cavity with a prevalence rate of about 0.5% to 2%.
The fact that distinguishes the Oral Lichen Planus (OLP) from other variants is that lesions inside the oral cavity rarely undergo spontaneous remission, whereas cutaneous lichen planus lesions are more or less self-limiting. Hence, early and accurate diagnosis becomes all the more essential to give symptomatic relief to the patients from the bothersome pain and sensitivity of the ulcerative or erosive lesions while it takes months to years for getting completely resolved.
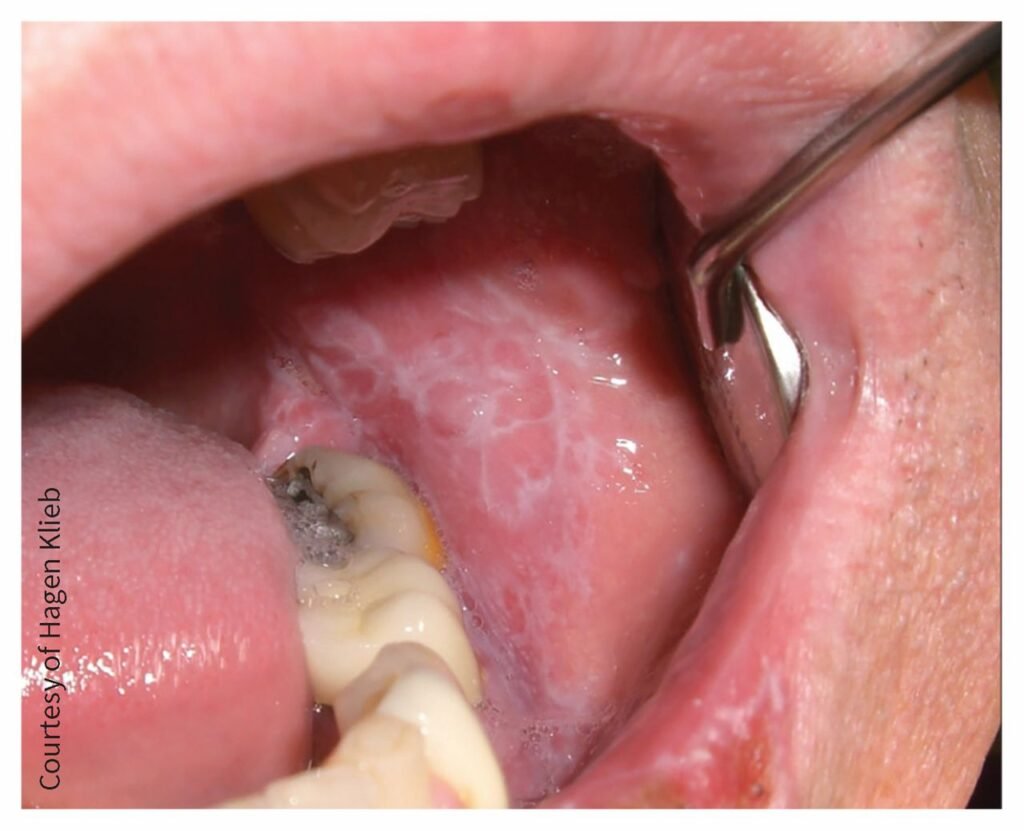
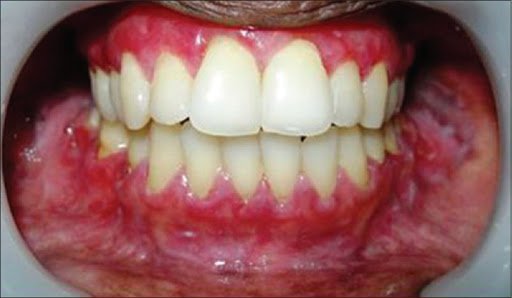
OLP Routine diagnosis relies upon the clinical picture and is confirmed by histopathology findings of the sample taken from oral lesions. But the results are often dubious and the disorder is repeatedly confused with non-specific inflammatory lesions, highlighting the need for improved detection methodologies.
Salivary biomarkers and oral biota have always played a crucial role in establishing the diagnosis of oral diseases. Recently, saliva-based testing of salivary cytokines and oral microbial flora has come forth as a potential diagnostic feature, assisting in differentiating the immune-mediated disease from inflammatory lesions economically and effortlessly.
The Research
Carvalho and colleagues from Brazil have researched about the potential role of our oral micobiota and salivary cytokines in telling apart Oran Lichen Planus (OLP) from Non-Specific Inflammatory Lesions (NSIL).
The aim of the study, published in Scientific Reports, a Nature Research journal, was to evaluate the genetic expression of various cytokines (small secreted proteins released by cells, which have a specific effect on the interactions and communications between cells) such as IFN-γ, IL-17 and IL-33 and oral microbial composition in samples taken from patients with OLP and in patients of NSIL of oral mucosa, analyzed as a control group.
The research group worked on 15 tissue samples obtained from patients with oral mucosal lesions. For finding the concentration and gene expression of cytokines the study required collection of Unstimulated whole saliva samples from the oral cavity which was accomplished with ease with the assistance of Super•SAL™-Universal Saliva Collection Kit Collection Device, Oasis Diagnostic Corporation.
The Sample Collection Device
Super-SAL has a user-friendly operating mechanism that takes the sample from a pool of saliva collected in the patient's mouth. The kit is a rapid and handy method for large volume sampling via a highly absorbent cylindrical-shaped pad. It has a built-in mechanism for sample sufficiency.
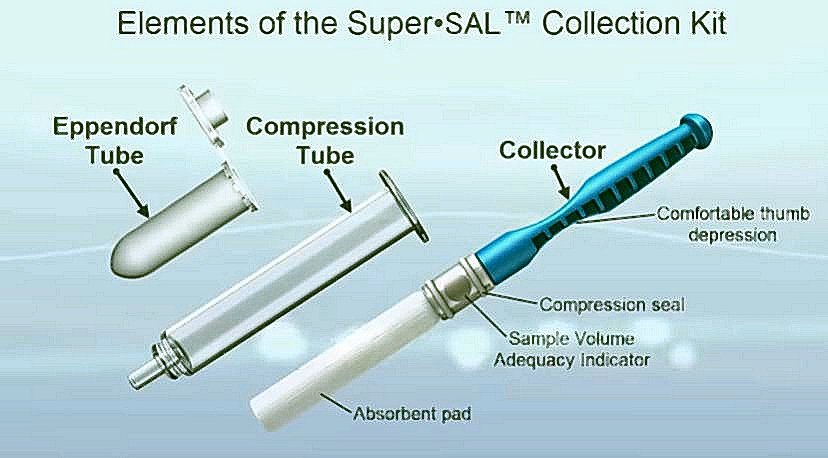
The volume adequacy indicator changes from yellow to blue when sufficient sample has been collected. The saliva is then separated very conveniently by compressing the absorbent pad used to collect the sample through a compression chamber and into a standard 2mL Eppendorf tube. A full-length video on the instructional use of the device can be accessed for insights here
The sample can be used immediately, sent to a laboratory for subsequent analysis or stabilized for later investigation. Supplementary information on the device can be found here
Applications
Effortless and non-invasive sample collection without any patient discomfort
Super•SAL™ being a universal sample collection kit has application in multiple fields and has been put in use for the collection of amniotic fluid, vaginal specimens, and urine specimens besides saliva samples
The kit has been used to collect saliva from multiple animal species such as cats, cows, pigs, horses, non-human primates, dogs, and humans
It has been brought to use to collect viruses, bacteria, hormones, proteins and certain drug molecules.
ABOUT OASIS DIAGNOSTICS- futuristic saliva-based technologies

Oasis Diagnostics ® Corporation was established in 2002 to address an urgent need and shortage of non-invasive saliva-based technology that would redefine the spectrum of sample collection, rapid testing and molecular diagnostics in the field of Life Sciences.
The company places confidence in early diagnostic strategies with an endeavour to disease prevention on a global basis.
OASIS DIAGNOSTICS is passionately working to stand up to the growing need for more effective screening tools, which may be applied to early detection of diseases and medical disorders, utilizing non-invasive test specimens with a particular interest in oral fluids (saliva) and development of rapid, point-of-care products, which fits into the Corporate sight of improving the quality of healthcare for the global citizens.
The Company’s entire range of futuristic diagnostic tools is covered by a portfolio of issued EU, US and International patents.
KROYNAS (Dr Kamalesh Roy Research and Diagnostics) Pvt. Ltd., the first and only start-up in India, focused specifically on dental Genetics and clinical medicine using saliva diagnostics and genomic technologies, is proud to exclusively represent Oasis Diagnostics in India.
Findings of The Study
Researchers noted that infections with several viruses were related to OLP, Also it has been previously established that Candida Albicans infection and Helicobacter Pylori infections are correlated with OLP.
The above all factors influence the oral microbial composition, consequently altering the local immunity and thus favouring the OLP progression.
The study also found that levels of, IFN-γ, a cytokine, in salivary samples was higher in OLP samples as compared to NSIL control samples. Also, higher genetic expression of IFN-γ was observed in OLP patients.
The Gist
Researchers have concluded that OLP lesions indicated a higher level of apoptotic cells, inflammatory infiltrate and a different microbiota when compared to NSIL. The results have brought forth essential points that add up as a criterion to the diagnosis and could be used as for a futuristic diagnostic tool.
Furthermore, considering that establishing the diagnosis of OLP is often a challenging procedure, it is thus imperative to underline that an accurate and reliable diagnosis would be better guided by taking into consideration a multitude of factors including the oral micro-biota and salivary cytokine levels.
Share your thoughts in the comments below. If you found this interesting, share it with your friends and follow our Facebook page @KROYNAS for more interesting info.
